Oral Paper Presentation
Annual Scientific Meeting
Session: Plenary Session 4A: Endoscopy / Esophagus
57 - Close, Coat, or Leave Alone? Evaluating Options to Reduce Delayed Bleeding in Endoscopic Submucosal Dissection
Wednesday, October 29, 2025
8:50 AM - 9:00 AM PDT
Location: North Ballroom 120D

Krystal Lai, MD
University of Texas Southwestern Medical Center
Dallas, TX
Presenting Author(s)
Krystal Lai, MD, Ronald C. Turner, MD, Garrett Ray, MD, Dyanna Gregory, MS, Lisa VanWagner, MD, MSc, Markus Goldschmiedt, MD, Thomas Tielleman, MD
University of Texas Southwestern Medical Center, Dallas, TX
Introduction: Endoscopic submucosal dissection (ESD) is a minimally invasive technique for resection of large lesions within the gastrointestinal (GI) tract. Delayed bleeding is a known potential complication. Data is mixed on whether prophylactic management of post-ESD defects, such as endoscopic closure or application of topical hemostatic agents, effectively reduces rates of delayed bleeding.
Methods: At an academic center with two large urban hospitals, all ESD cases between July 2020 and April 2025 were identified via retrospective chart review. Patients received one of three types of post-ESD defect management as bleeding prophylaxis: thermal, closure, or self-assembling peptide (SAP). All patients received thermal coagulation of visible vessels in the resection bed. Thermal prophylaxis included no additional interventions. Closure prophylaxis included additional closure of the defect with endoscopic clips and/or sutures. SAP prophylaxis included additional application of a synthetic SAP hemostatic gel to the defect. Delayed bleeding was defined as overt GI bleeding symptoms requiring endoscopy or leading to > 2 g/dL decline in hemoglobin within 30 days of procedure. Univariate analysis and clinical significance were used to select covariates for multivariable logistic regression models, which were fit to generate adjusted odds ratios for the probability of delayed bleeding after ESD.
Results: Of the 352 ESD cases identified, 96 (27.3%) received thermal prophylaxis, 185 (52.6%) received closure prophylaxis, and 71 (20.2%) received SAP prophylaxis. In total, 15 cases (4.3%) resulted in delayed bleeding, occurring in 4/96 (4.2%) thermal cases, 9/185 (4.9%) closure cases, and 2/71 (2.8%) SAP cases. After adjusting for medical comorbidities, use of antithrombotic agents, and procedural characteristics, there was no statistical difference in rates of delayed bleeding when comparing closure (OR 1.51, 95% CI 0.39 - 5.95) or SAP (OR 0.78, 95% CI 0.12 - 5.29) to thermal prophylaxis. Even within the high-risk sub-groups of patients on antiplatelet agents or with resection diameter > 50 mm, there was still no statistical difference between management approaches (Table 1).
Discussion: There is no evidence to suggest that additional prophylaxis, including either endoscopic closure of post-ESD defect or use of SAP, improves rates of delayed bleeding compared to thermal prophylaxis alone. Future large prospective studies may assist in further confirming the outcomes of this retrospective study.
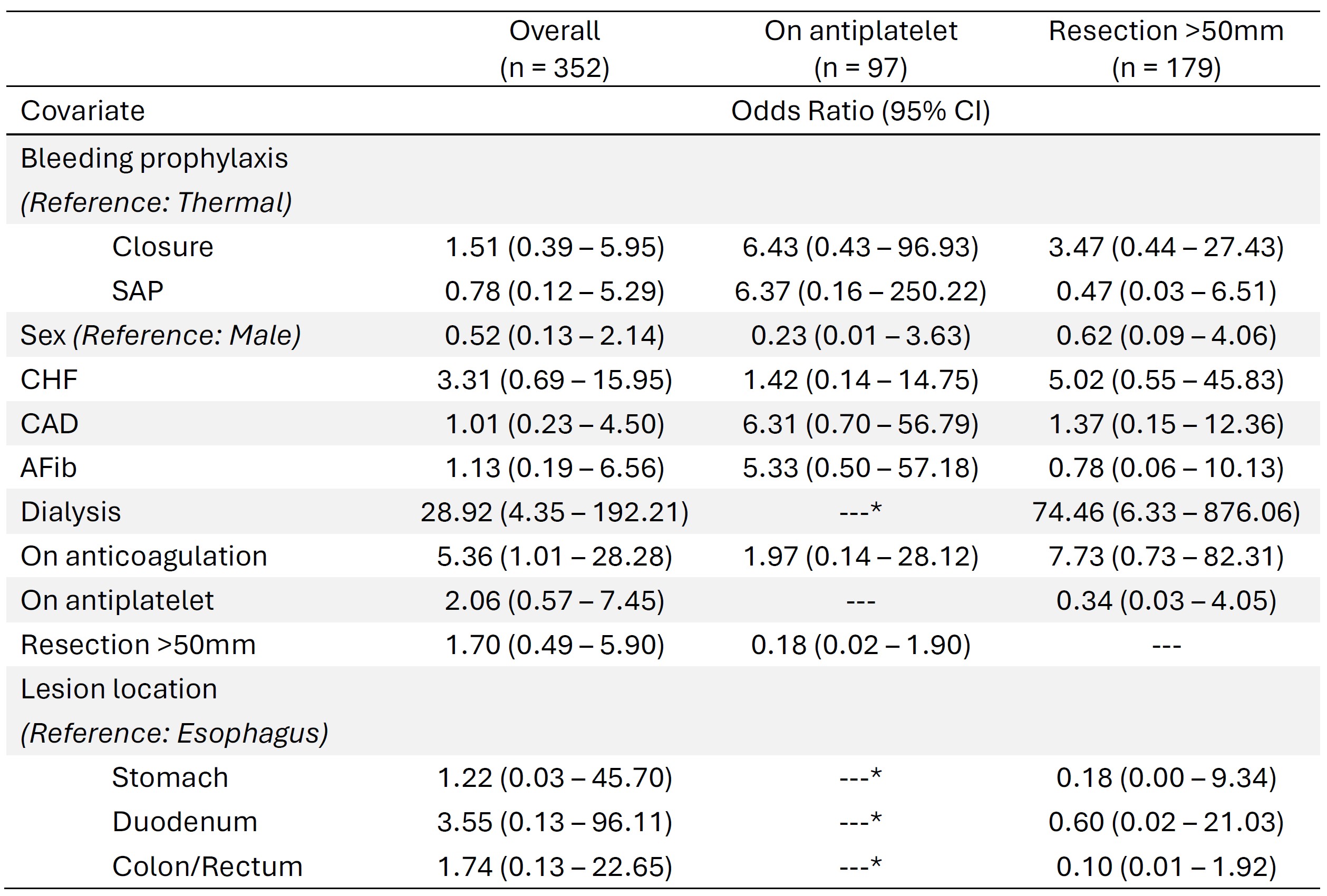
Figure: Table 1: Multivariable logistic regression analysis with odds ratios for delayed bleeding in the overall population and high-risk subgroups. On anticoagulation = patients on a direct oral anticoagulant or warfarin; On antiplatelet = patients on aspirin, clopidogrel, or dual antiplatelet therapy; Resection >50mm = patients with resection diameter greater than 50 millimeters; CI = confidence interval; SAP = self-assembling peptide; CHF = congestive heart failure; CAD = coronary artery disease; AFib = atrial fibrillation; *These covariates were removed from the model due to low frequency
Disclosures:
Krystal Lai indicated no relevant financial relationships.
Ronald Turner indicated no relevant financial relationships.
Garrett Ray indicated no relevant financial relationships.
Dyanna Gregory indicated no relevant financial relationships.
Lisa VanWagner: Alpha Insights – Consultant. Gerson Lehrman Group – Consultant. Madrigal Pharmaceutical – Advisory Committee/Board Member, Grant/Research Support. Slingshot Insights – Consultant. W.L. Gore & Associates – Grant/Research Support.
Markus Goldschmiedt indicated no relevant financial relationships.
Thomas Tielleman: ConMed – Consultant.
Krystal Lai, MD, Ronald C. Turner, MD, Garrett Ray, MD, Dyanna Gregory, MS, Lisa VanWagner, MD, MSc, Markus Goldschmiedt, MD, Thomas Tielleman, MD, 57, Close, Coat, or Leave Alone? Evaluating Options to Reduce Delayed Bleeding in Endoscopic Submucosal Dissection, ACG 2025 Annual Scientific Meeting Abstracts. Phoenix, AZ: American College of Gastroenterology.
University of Texas Southwestern Medical Center, Dallas, TX
Introduction: Endoscopic submucosal dissection (ESD) is a minimally invasive technique for resection of large lesions within the gastrointestinal (GI) tract. Delayed bleeding is a known potential complication. Data is mixed on whether prophylactic management of post-ESD defects, such as endoscopic closure or application of topical hemostatic agents, effectively reduces rates of delayed bleeding.
Methods: At an academic center with two large urban hospitals, all ESD cases between July 2020 and April 2025 were identified via retrospective chart review. Patients received one of three types of post-ESD defect management as bleeding prophylaxis: thermal, closure, or self-assembling peptide (SAP). All patients received thermal coagulation of visible vessels in the resection bed. Thermal prophylaxis included no additional interventions. Closure prophylaxis included additional closure of the defect with endoscopic clips and/or sutures. SAP prophylaxis included additional application of a synthetic SAP hemostatic gel to the defect. Delayed bleeding was defined as overt GI bleeding symptoms requiring endoscopy or leading to > 2 g/dL decline in hemoglobin within 30 days of procedure. Univariate analysis and clinical significance were used to select covariates for multivariable logistic regression models, which were fit to generate adjusted odds ratios for the probability of delayed bleeding after ESD.
Results: Of the 352 ESD cases identified, 96 (27.3%) received thermal prophylaxis, 185 (52.6%) received closure prophylaxis, and 71 (20.2%) received SAP prophylaxis. In total, 15 cases (4.3%) resulted in delayed bleeding, occurring in 4/96 (4.2%) thermal cases, 9/185 (4.9%) closure cases, and 2/71 (2.8%) SAP cases. After adjusting for medical comorbidities, use of antithrombotic agents, and procedural characteristics, there was no statistical difference in rates of delayed bleeding when comparing closure (OR 1.51, 95% CI 0.39 - 5.95) or SAP (OR 0.78, 95% CI 0.12 - 5.29) to thermal prophylaxis. Even within the high-risk sub-groups of patients on antiplatelet agents or with resection diameter > 50 mm, there was still no statistical difference between management approaches (Table 1).
Discussion: There is no evidence to suggest that additional prophylaxis, including either endoscopic closure of post-ESD defect or use of SAP, improves rates of delayed bleeding compared to thermal prophylaxis alone. Future large prospective studies may assist in further confirming the outcomes of this retrospective study.

Figure: Table 1: Multivariable logistic regression analysis with odds ratios for delayed bleeding in the overall population and high-risk subgroups. On anticoagulation = patients on a direct oral anticoagulant or warfarin; On antiplatelet = patients on aspirin, clopidogrel, or dual antiplatelet therapy; Resection >50mm = patients with resection diameter greater than 50 millimeters; CI = confidence interval; SAP = self-assembling peptide; CHF = congestive heart failure; CAD = coronary artery disease; AFib = atrial fibrillation; *These covariates were removed from the model due to low frequency
Disclosures:
Krystal Lai indicated no relevant financial relationships.
Ronald Turner indicated no relevant financial relationships.
Garrett Ray indicated no relevant financial relationships.
Dyanna Gregory indicated no relevant financial relationships.
Lisa VanWagner: Alpha Insights – Consultant. Gerson Lehrman Group – Consultant. Madrigal Pharmaceutical – Advisory Committee/Board Member, Grant/Research Support. Slingshot Insights – Consultant. W.L. Gore & Associates – Grant/Research Support.
Markus Goldschmiedt indicated no relevant financial relationships.
Thomas Tielleman: ConMed – Consultant.
Krystal Lai, MD, Ronald C. Turner, MD, Garrett Ray, MD, Dyanna Gregory, MS, Lisa VanWagner, MD, MSc, Markus Goldschmiedt, MD, Thomas Tielleman, MD, 57, Close, Coat, or Leave Alone? Evaluating Options to Reduce Delayed Bleeding in Endoscopic Submucosal Dissection, ACG 2025 Annual Scientific Meeting Abstracts. Phoenix, AZ: American College of Gastroenterology.


