Oral Paper Presentation
Annual Scientific Meeting
Session: Plenary Session 2B: Liver / Biliary / Pancreas / Endoscopy
33 - "Early Is Not Always Better": Impact of Endoscopy Timing in Cirrhotic Patients with Acute Variceal Bleeding - An Updated Systematic Review and Meta-Analysis
Tuesday, October 28, 2025
9:20 AM - 9:30 AM PDT
Location: North Ballroom 120BC

Anchit Chauhan (he/him/his)
Maulana Azad Medical College
New Delhi, Delhi, India
Presenting Author(s)
Award: ACG International Award
Adnan Bhat, MD1, Anchit Chauhan, 2, Muhammad Hamza, MBBS3, Marium Zahid, 4, Asad Iqbal, 5, Marhaba Fatima, 6, Saniya Ishtiaq, 7, Kinza Jawed, MBBS8, Ayesha Arshad, MBBS9, Mariam Shahabi, MBBS9, Omar Al-Radideh, MD10
1University of Florida, Gainesville, FL; 2Maulana Azad Medical College, New Delhi, Delhi, India; 3Saidu medical college swat, Saidu Sharif, North-West Frontier, Pakistan; 4Karachi Medical and Dental College, Karachi, Sindh, Pakistan; 5Bacha Khan Medical College, Mardan, North-West Frontier, Pakistan; 6People’s University of Medical and Health Sciences for Women, Nawabshah, Sindh, Pakistan; 7Rawalpindi Medical University, Rawalpindi, Pakistan, Rawalpindi, Punjab, Pakistan; 8Aga Khan University, Karachi, Sindh, Pakistan; 9Dow Medical College, Karachi, Sindh, Pakistan; 10University of Florida College of Medicine, Gainesville, FL
Introduction: The optimal timing of endoscopy in cirrhotic patients with acute variceal bleeding (AVB) remains controversial, with contradictory results from recent studies. This updated meta-analysis incorporates newer, higher-quality evidence since the last similar analysis (Bai 2021), to clarify the impact of endoscopic timing on patient outcomes.
Methods: Following PRISMA guidelines (PROSPERO: CRD420251063584), PubMed, Scopus, Cochrane CENTRAL, and Embase were searched by two reviewers. We included observational studies and clinical trials comparing early versus delayed endoscopy based on timing from admission to endoscopy (≤6h, ≤12h, ≤48h). We defined very early endoscopy as ≤6h and early endoscopy as ≤12h from admission. Outcomes included all-cause mortality, rebleeding, and adverse events (AEs, like perforation, infection, aspiration). Results were pooled using RevMan 5.4.1, random-effects model (p< 0.05 for significance). A priori subgroup analyses (mortality: 6 week/in-hospital and rebleeding: early/delayed/undefined), sensitivity analyses, and Egger's tests were conducted to address bias.
Results: 15 studies (11 retrospective, 3 prospective, 1 RCT; N=9,046 patients, >3x prior meta-analyses) were included. Endoscopy within 48h significantly reduced all-cause mortality vs >48h (RR 0.53, 95% CI 0.30-0.94, I2= 26%). In contrast, very early endoscopy (≤6h) was associated with increased mortality (RR 1.57, 95% CI 1.05-2.34, I2 = 0%). Early endoscopy (≤12h) showed no mortality benefit. In-hospital mortality was also lower with endoscopy ≤48h (RR 0.56, 95% CI 0.34-0.92, I2=15%) [Figure 1]. Rebleeding rates did not differ overall or by subgroup. However, early endoscopy (≤12h) significantly increased overall AEs (RR 2.98, 95% CI 1.83-4.84, p< 0.0001, I2=5%) [Figure 2].
Discussion: Endoscopy within 48h reduces overall and in-hospital mortality in cirrhotic AVB. However, very early endoscopy (≤6h) may increase mortality—possibly due to inadequate stabilization or selection bias. Early timing also increases AEs, highlighting the need for individualized decision-making. Unlike prior analyses that pooled heterogeneous thresholds, our study clearly defines very-early and early timing and presents low-heterogeneity evidence. These findings challenge the "early is always better" paradigm and support a more nuanced approach to endoscopy timing in AVB.
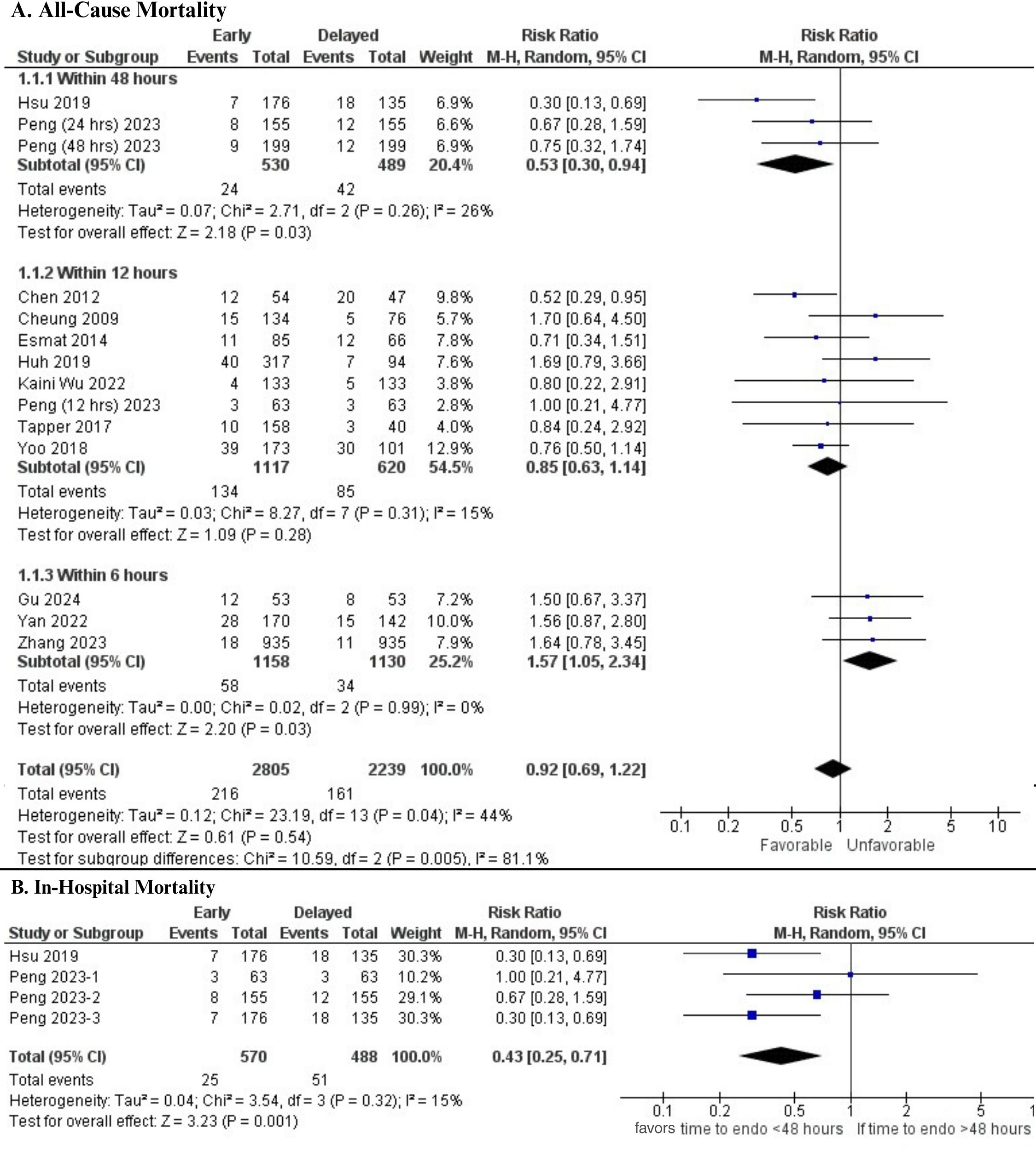
Figure: Forest Plot of Mortality Outcomes: Subgroup Analyses by Endoscopy Timing and In-Hospital Mortality
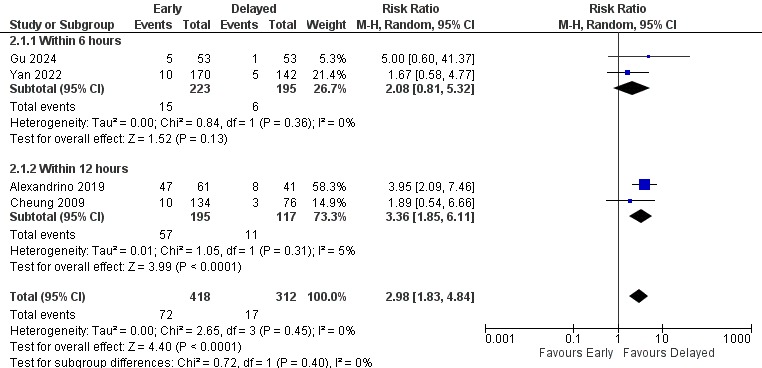
Figure: Figure 2: Forest Plot of Overall Adverse Events Outcome
Disclosures:
Adnan Bhat indicated no relevant financial relationships.
Anchit Chauhan indicated no relevant financial relationships.
Muhammad Hamza indicated no relevant financial relationships.
Marium Zahid indicated no relevant financial relationships.
Asad Iqbal indicated no relevant financial relationships.
Marhaba Fatima indicated no relevant financial relationships.
Saniya Ishtiaq indicated no relevant financial relationships.
Kinza Jawed indicated no relevant financial relationships.
Ayesha Arshad indicated no relevant financial relationships.
Mariam Shahabi indicated no relevant financial relationships.
Omar Al-Radideh indicated no relevant financial relationships.
Adnan Bhat, MD1, Anchit Chauhan, 2, Muhammad Hamza, MBBS3, Marium Zahid, 4, Asad Iqbal, 5, Marhaba Fatima, 6, Saniya Ishtiaq, 7, Kinza Jawed, MBBS8, Ayesha Arshad, MBBS9, Mariam Shahabi, MBBS9, Omar Al-Radideh, MD10, 33, "Early Is Not Always Better": Impact of Endoscopy Timing in Cirrhotic Patients with Acute Variceal Bleeding - An Updated Systematic Review and Meta-Analysis, ACG 2025 Annual Scientific Meeting Abstracts. Phoenix, AZ: American College of Gastroenterology.
Adnan Bhat, MD1, Anchit Chauhan, 2, Muhammad Hamza, MBBS3, Marium Zahid, 4, Asad Iqbal, 5, Marhaba Fatima, 6, Saniya Ishtiaq, 7, Kinza Jawed, MBBS8, Ayesha Arshad, MBBS9, Mariam Shahabi, MBBS9, Omar Al-Radideh, MD10
1University of Florida, Gainesville, FL; 2Maulana Azad Medical College, New Delhi, Delhi, India; 3Saidu medical college swat, Saidu Sharif, North-West Frontier, Pakistan; 4Karachi Medical and Dental College, Karachi, Sindh, Pakistan; 5Bacha Khan Medical College, Mardan, North-West Frontier, Pakistan; 6People’s University of Medical and Health Sciences for Women, Nawabshah, Sindh, Pakistan; 7Rawalpindi Medical University, Rawalpindi, Pakistan, Rawalpindi, Punjab, Pakistan; 8Aga Khan University, Karachi, Sindh, Pakistan; 9Dow Medical College, Karachi, Sindh, Pakistan; 10University of Florida College of Medicine, Gainesville, FL
Introduction: The optimal timing of endoscopy in cirrhotic patients with acute variceal bleeding (AVB) remains controversial, with contradictory results from recent studies. This updated meta-analysis incorporates newer, higher-quality evidence since the last similar analysis (Bai 2021), to clarify the impact of endoscopic timing on patient outcomes.
Methods: Following PRISMA guidelines (PROSPERO: CRD420251063584), PubMed, Scopus, Cochrane CENTRAL, and Embase were searched by two reviewers. We included observational studies and clinical trials comparing early versus delayed endoscopy based on timing from admission to endoscopy (≤6h, ≤12h, ≤48h). We defined very early endoscopy as ≤6h and early endoscopy as ≤12h from admission. Outcomes included all-cause mortality, rebleeding, and adverse events (AEs, like perforation, infection, aspiration). Results were pooled using RevMan 5.4.1, random-effects model (p< 0.05 for significance). A priori subgroup analyses (mortality: 6 week/in-hospital and rebleeding: early/delayed/undefined), sensitivity analyses, and Egger's tests were conducted to address bias.
Results: 15 studies (11 retrospective, 3 prospective, 1 RCT; N=9,046 patients, >3x prior meta-analyses) were included. Endoscopy within 48h significantly reduced all-cause mortality vs >48h (RR 0.53, 95% CI 0.30-0.94, I2= 26%). In contrast, very early endoscopy (≤6h) was associated with increased mortality (RR 1.57, 95% CI 1.05-2.34, I2 = 0%). Early endoscopy (≤12h) showed no mortality benefit. In-hospital mortality was also lower with endoscopy ≤48h (RR 0.56, 95% CI 0.34-0.92, I2=15%) [Figure 1]. Rebleeding rates did not differ overall or by subgroup. However, early endoscopy (≤12h) significantly increased overall AEs (RR 2.98, 95% CI 1.83-4.84, p< 0.0001, I2=5%) [Figure 2].
Discussion: Endoscopy within 48h reduces overall and in-hospital mortality in cirrhotic AVB. However, very early endoscopy (≤6h) may increase mortality—possibly due to inadequate stabilization or selection bias. Early timing also increases AEs, highlighting the need for individualized decision-making. Unlike prior analyses that pooled heterogeneous thresholds, our study clearly defines very-early and early timing and presents low-heterogeneity evidence. These findings challenge the "early is always better" paradigm and support a more nuanced approach to endoscopy timing in AVB.

Figure: Forest Plot of Mortality Outcomes: Subgroup Analyses by Endoscopy Timing and In-Hospital Mortality

Figure: Figure 2: Forest Plot of Overall Adverse Events Outcome
Disclosures:
Adnan Bhat indicated no relevant financial relationships.
Anchit Chauhan indicated no relevant financial relationships.
Muhammad Hamza indicated no relevant financial relationships.
Marium Zahid indicated no relevant financial relationships.
Asad Iqbal indicated no relevant financial relationships.
Marhaba Fatima indicated no relevant financial relationships.
Saniya Ishtiaq indicated no relevant financial relationships.
Kinza Jawed indicated no relevant financial relationships.
Ayesha Arshad indicated no relevant financial relationships.
Mariam Shahabi indicated no relevant financial relationships.
Omar Al-Radideh indicated no relevant financial relationships.
Adnan Bhat, MD1, Anchit Chauhan, 2, Muhammad Hamza, MBBS3, Marium Zahid, 4, Asad Iqbal, 5, Marhaba Fatima, 6, Saniya Ishtiaq, 7, Kinza Jawed, MBBS8, Ayesha Arshad, MBBS9, Mariam Shahabi, MBBS9, Omar Al-Radideh, MD10, 33, "Early Is Not Always Better": Impact of Endoscopy Timing in Cirrhotic Patients with Acute Variceal Bleeding - An Updated Systematic Review and Meta-Analysis, ACG 2025 Annual Scientific Meeting Abstracts. Phoenix, AZ: American College of Gastroenterology.


