Oral Paper Presentation
Annual Scientific Meeting
Session: Plenary Session 2A: Colon / IBD / Practice Management
23 - Virtual Multidisciplinary GI Clinic Improves Patient Engagement, Satisfaction, and Symptoms at Reduced Costs and Healthcare Utilization: A Propensity-Matched Prospective Observational Study
Tuesday, October 28, 2025
9:10 AM - 9:20 AM PDT
Location: North Ballroom 120D
.jpg)
Sameer K. Berry, MD, MBA
Clinical Assistant Professor
NYU Langone Health
Los Angeles, CA
Presenting Author(s)
Sameer Berry, MD1, Sanskriti Varma, MD2, Chamara Basnayake, MBBS3, Jeffrey Berinstein, MD, MS4, Walter Chan, MD, MPH, FACG5, John Allen, MD, MBA4, William Chey, MD, FACG4
1NYU Langone Health, New York, NY; 2Massachusetts General Hospital, Somerville, MA; 3St Vincent’s Hospital Melbourne – Department of Gastroenterology, Melbourne, Victoria, Australia; 4University of Michigan Health, Ann Arbor, MI; 5Brigham and Women's Hospital, Boston, MA
Introduction: Gastrointestinal (GI) disorders are common, burdensome, and costly. Virtual and multidisciplinary models each improve outcomes, yet no study has tested a virtual multidisciplinary clinic for GI care. We evaluated the impact of a virtual multidisciplinary GI clinic on patient-reported outcomes, utilization, and costs.
Methods: This is a prospective observational study of adults with commercial insurance who enrolled in a virtual, multidisciplinary gastroenterology clinic between 3/2021-5/2025. Patients receiving ≥1 year of care were analyzed for clinical engagement. Patients who completed ≥4 clinical visits provided self-reported outcomes at baseline and after the most recent visit, including symptom severity, global symptom control, and satisfaction. McNemar’s Chi-square tests assessed paired pre-post outcomes. Claims data from 9- and 12-month periods were compared to propensity-matched controls using difference-in-difference (DiD) analysis, adjusting for baseline clinical and cost factors.
Results: We included 2,796 patients (65% female, mean age 40±11 years) and 3,102 matched controls. Among clinic patients, the most common GI conditions were disorders of gut brain interaction (49%) and esophageal disorders (38%, Table 1), with new GI diagnoses made in 36%. Enrolled patients completed a mean of 7 visits (range 1–46) and exchanged an average of 61 messages (range 5–942). Most patients received care from dietitians (82%) and GI psychologists (56%). Significant improvements were observed in symptom severity (n=1,246; 28% moderate-to-severe post-care vs. 78% at baseline; p< 0.0001), global symptom control (n=1,315; 90% post-care vs. 14% at baseline; p< 0.0001), and satisfaction with care (n=460; 97% satisfied post-care vs. 30% at baseline; p< 0.0001, Table 2). Compared to matched controls, there were significant reductions in GI-ED visits (68%, p< 0.0001), GI-surgery (56%, p=0.02), GI-inpatient admissions (52%, p=0.05), and GI-imaging (50%, p< 0.0001) at 9 months post-enrollment. All-cause costs were substantially reduced at 9 months ($10,700 vs. $15,275; DiD = $5,788; p< 0.0001) and remained significantly lower at 12 months ($14,412 vs. $19,449; DiD = $6,081; p=0.002).
Discussion: A fully virtual multidisciplinary GI clinic yielded high clinical engagement, improved symptoms and satisfaction, and markedly lowered utilization and costs, supporting its scalability for modern GI care.
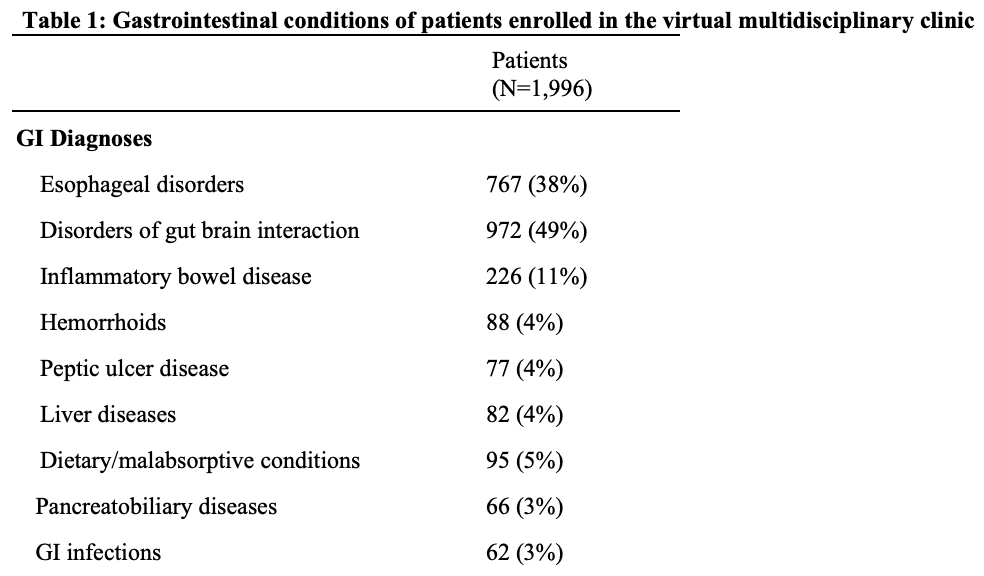
Figure: Values shown as N (%) or mean (standard deviation) for patients with documented diagnoses. Patients can have more than one condition and be classified multiple times. Diagnosis data is reflective of members who remained engaged in the clinic for at least 1 year.
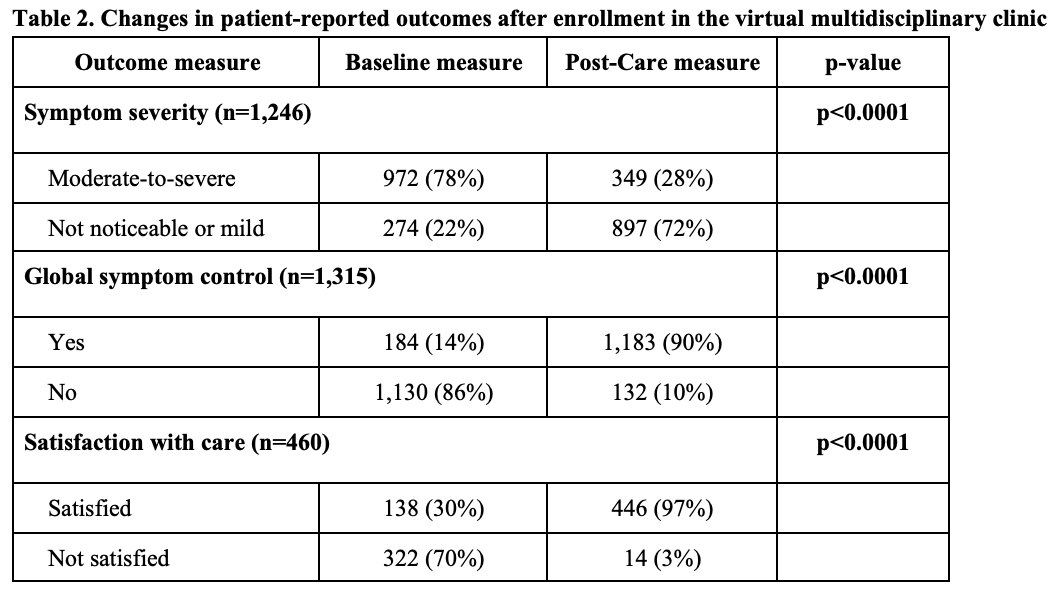
Figure: Symptom severity was assessed using a non-validated clinical questionnaire developed by Oshi Health for internal clinical use, and measured in the following categories: not noticeable, mild, moderate, severe. For the purposes of analyses, responses were grouped into “moderate/severe” or “not noticeable/mild”.
Global symptom control was assessed using a non-validated clinical questionnaire developed by Oshi Health for internal clinical use and measured in the following categories: yes, no.
Satisfaction with care was measured using the validated Customer Satisfaction Survey in the following categories: very dissatisfied, dissatisfied, neutral, satisfied, very satisfied. For the purposes of analyses, responses were grouped into “satisfied” if patients reported “satisfied” or “very satisfied” and “not satisfied” if patients reported “neutral”, “dissatisfied”, or “very dissatisfied”.
Disclosures:
Sameer Berry: Oshi Health – Employee.
Sanskriti Varma: Oshi Health – Consultant.
Chamara Basnayake indicated no relevant financial relationships.
Jeffrey Berinstein indicated no relevant financial relationships.
Walter Chan indicated no relevant financial relationships.
John Allen indicated no relevant financial relationships.
William Chey: Ardelyx – Consultant. Atmo – Consultant. Biomerica – Consultant. Commonwealth Diagnostics International – Grant/Research Support. Coprata – Stock Options. Dieta – Stock Options. Digital Manometry – Intellectual Property/Patents. Evinature – Stock Options. FoodMarble – Stock Options. Gemelli – Consultant. Kiwi BioScience – Stock Options. Modify Health – Stock Options. My Nutrition Health – Intellectual Property/Patents. Phathom – Consultant. Rectal Expulsion Device – Intellectual Property/Patents. Redhill – Consultant. Salix – Consultant, Grant/Research Support. Takeda – Consultant. Vibrant – Consultant.
Sameer Berry, MD1, Sanskriti Varma, MD2, Chamara Basnayake, MBBS3, Jeffrey Berinstein, MD, MS4, Walter Chan, MD, MPH, FACG5, John Allen, MD, MBA4, William Chey, MD, FACG4, 23, Virtual Multidisciplinary GI Clinic Improves Patient Engagement, Satisfaction, and Symptoms at Reduced Costs and Healthcare Utilization: A Propensity-Matched Prospective Observational Study, ACG 2025 Annual Scientific Meeting Abstracts. Phoenix, AZ: American College of Gastroenterology.
1NYU Langone Health, New York, NY; 2Massachusetts General Hospital, Somerville, MA; 3St Vincent’s Hospital Melbourne – Department of Gastroenterology, Melbourne, Victoria, Australia; 4University of Michigan Health, Ann Arbor, MI; 5Brigham and Women's Hospital, Boston, MA
Introduction: Gastrointestinal (GI) disorders are common, burdensome, and costly. Virtual and multidisciplinary models each improve outcomes, yet no study has tested a virtual multidisciplinary clinic for GI care. We evaluated the impact of a virtual multidisciplinary GI clinic on patient-reported outcomes, utilization, and costs.
Methods: This is a prospective observational study of adults with commercial insurance who enrolled in a virtual, multidisciplinary gastroenterology clinic between 3/2021-5/2025. Patients receiving ≥1 year of care were analyzed for clinical engagement. Patients who completed ≥4 clinical visits provided self-reported outcomes at baseline and after the most recent visit, including symptom severity, global symptom control, and satisfaction. McNemar’s Chi-square tests assessed paired pre-post outcomes. Claims data from 9- and 12-month periods were compared to propensity-matched controls using difference-in-difference (DiD) analysis, adjusting for baseline clinical and cost factors.
Results: We included 2,796 patients (65% female, mean age 40±11 years) and 3,102 matched controls. Among clinic patients, the most common GI conditions were disorders of gut brain interaction (49%) and esophageal disorders (38%, Table 1), with new GI diagnoses made in 36%. Enrolled patients completed a mean of 7 visits (range 1–46) and exchanged an average of 61 messages (range 5–942). Most patients received care from dietitians (82%) and GI psychologists (56%). Significant improvements were observed in symptom severity (n=1,246; 28% moderate-to-severe post-care vs. 78% at baseline; p< 0.0001), global symptom control (n=1,315; 90% post-care vs. 14% at baseline; p< 0.0001), and satisfaction with care (n=460; 97% satisfied post-care vs. 30% at baseline; p< 0.0001, Table 2). Compared to matched controls, there were significant reductions in GI-ED visits (68%, p< 0.0001), GI-surgery (56%, p=0.02), GI-inpatient admissions (52%, p=0.05), and GI-imaging (50%, p< 0.0001) at 9 months post-enrollment. All-cause costs were substantially reduced at 9 months ($10,700 vs. $15,275; DiD = $5,788; p< 0.0001) and remained significantly lower at 12 months ($14,412 vs. $19,449; DiD = $6,081; p=0.002).
Discussion: A fully virtual multidisciplinary GI clinic yielded high clinical engagement, improved symptoms and satisfaction, and markedly lowered utilization and costs, supporting its scalability for modern GI care.

Figure: Values shown as N (%) or mean (standard deviation) for patients with documented diagnoses. Patients can have more than one condition and be classified multiple times. Diagnosis data is reflective of members who remained engaged in the clinic for at least 1 year.

Figure: Symptom severity was assessed using a non-validated clinical questionnaire developed by Oshi Health for internal clinical use, and measured in the following categories: not noticeable, mild, moderate, severe. For the purposes of analyses, responses were grouped into “moderate/severe” or “not noticeable/mild”.
Global symptom control was assessed using a non-validated clinical questionnaire developed by Oshi Health for internal clinical use and measured in the following categories: yes, no.
Satisfaction with care was measured using the validated Customer Satisfaction Survey in the following categories: very dissatisfied, dissatisfied, neutral, satisfied, very satisfied. For the purposes of analyses, responses were grouped into “satisfied” if patients reported “satisfied” or “very satisfied” and “not satisfied” if patients reported “neutral”, “dissatisfied”, or “very dissatisfied”.
Disclosures:
Sameer Berry: Oshi Health – Employee.
Sanskriti Varma: Oshi Health – Consultant.
Chamara Basnayake indicated no relevant financial relationships.
Jeffrey Berinstein indicated no relevant financial relationships.
Walter Chan indicated no relevant financial relationships.
John Allen indicated no relevant financial relationships.
William Chey: Ardelyx – Consultant. Atmo – Consultant. Biomerica – Consultant. Commonwealth Diagnostics International – Grant/Research Support. Coprata – Stock Options. Dieta – Stock Options. Digital Manometry – Intellectual Property/Patents. Evinature – Stock Options. FoodMarble – Stock Options. Gemelli – Consultant. Kiwi BioScience – Stock Options. Modify Health – Stock Options. My Nutrition Health – Intellectual Property/Patents. Phathom – Consultant. Rectal Expulsion Device – Intellectual Property/Patents. Redhill – Consultant. Salix – Consultant, Grant/Research Support. Takeda – Consultant. Vibrant – Consultant.
Sameer Berry, MD1, Sanskriti Varma, MD2, Chamara Basnayake, MBBS3, Jeffrey Berinstein, MD, MS4, Walter Chan, MD, MPH, FACG5, John Allen, MD, MBA4, William Chey, MD, FACG4, 23, Virtual Multidisciplinary GI Clinic Improves Patient Engagement, Satisfaction, and Symptoms at Reduced Costs and Healthcare Utilization: A Propensity-Matched Prospective Observational Study, ACG 2025 Annual Scientific Meeting Abstracts. Phoenix, AZ: American College of Gastroenterology.


